Home vs. Portable: Can One Oxygen Concentrator Do Both?
Home vs. Portable: Can One Oxygen Concentrator Do Both?
For many Australians managing chronic respiratory conditions like COPD or emphysema, the quest for the “perfect” oxygen setup often leads to one critical question: Can one oxygen concentrator do both home and portable tasks? The prospect of buying a single, versatile device is incredibly appealing. It suggests lower upfront costs, less maintenance, and a simplified lifestyle. However, when comparing a home oxygen concentrator vs. portable units, the reality of “all-in-one” solutions is often more complex than it appears on the surface.
In this guide, we will break down the technical differences between stationary and mobile units, evaluate the feasibility of “hybrid” devices, and help you determine which setup offers the best value for your health and your wallet.
See more: Home vs. Portable: Can One Oxygen Concentrator Do Both?
Understanding the Core Differences: Stationary vs. Mobile
To understand if one device can “do it all,” we must first define what these machines are engineered to achieve.
What is a Stationary Oxygen Unit?
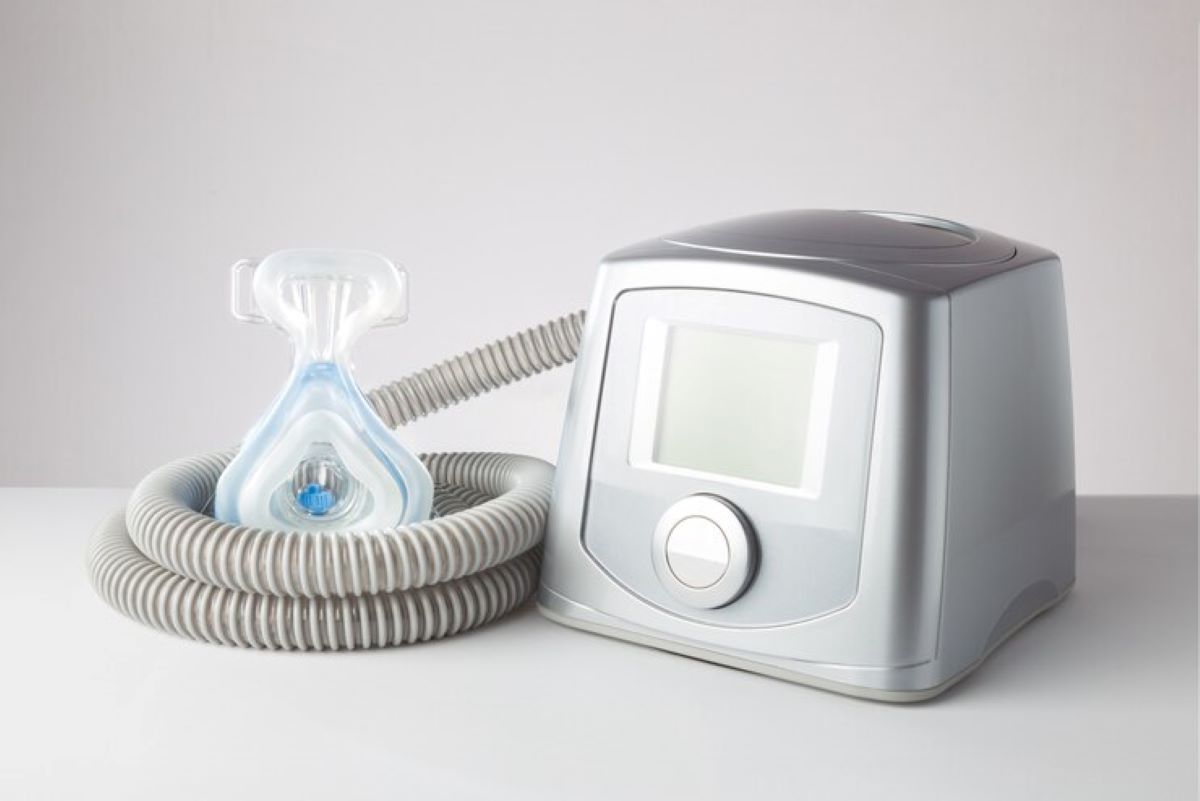
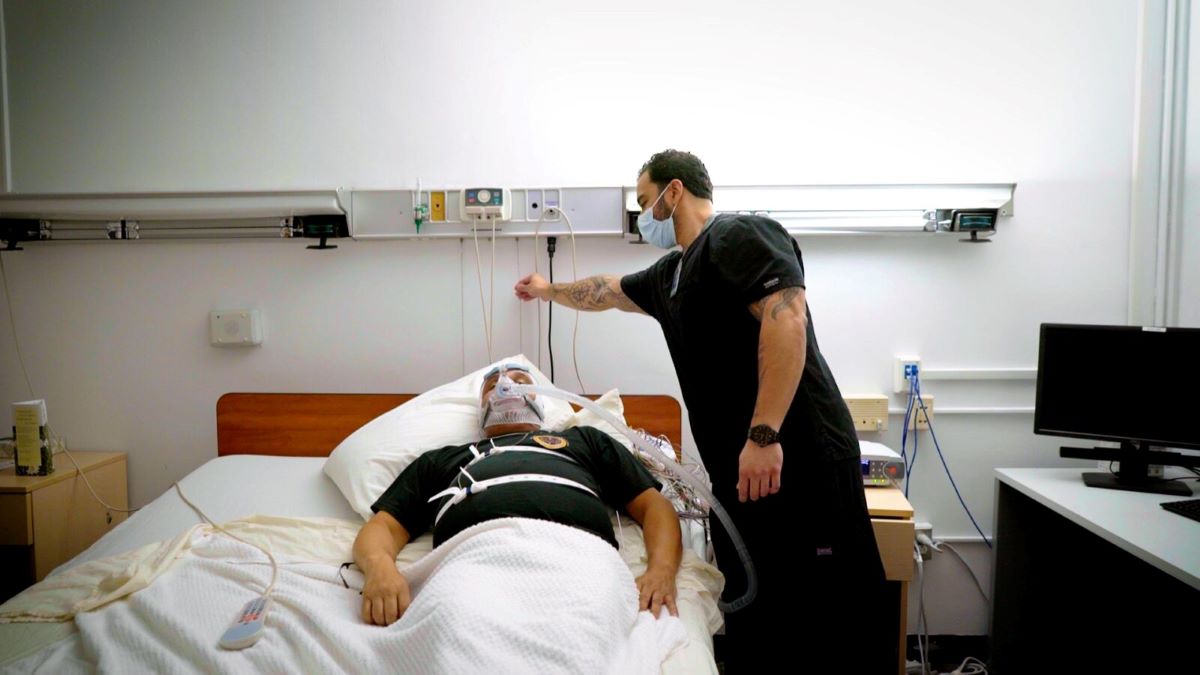
A stationary or home oxygen concentrator is a powerhouse. These units are designed to run 24/7, drawing in room air, removing nitrogen, and delivering medical-grade oxygen via a long nasal cannula.
- Output: Usually 5 to 10 litres per minute (LPM).
- Delivery: Continuous flow (a steady stream of oxygen).
- Power: Plugs directly into a wall outlet (AC power).
- Weight: Often 14kg to 25kg, moved on castor wheels.
What is a Portable Oxygen Concentrator (POC)?
A portable oxygen concentrator is built for mobility. These devices are lightweight and battery-operated, allowing users to leave the house, attend social events, or travel on planes.
- Output: Typically measured in “settings” rather than raw LPM.
- Delivery: Most use “Pulse Dose” (bursts of oxygen triggered by inhalation).
- Power: Rechargeable lithium-ion batteries and DC (car) adapters.
- Weight: Ranges from 1kg to 8kg.
The Concept of All-in-One Oxygen Solutions
Can you actually find a device that bridges this gap? Technically, yes. There are “continuous flow” portable units that aim to serve as all-in-one oxygen solutions.
However, these devices are a compromise by design. They are larger than standard pulse-dose portables but smaller than home units. While they can be used at home and in a car, they are often too heavy (approx. 8kg) for a stroll through the park and may lack the high-capacity compressors found in dedicated home units.
The Trade-offs of a Single-Unit Strategy
- Mechanical Wear: A home unit is built for 20,000+ hours of run time. Using a portable unit as your primary home source significantly accelerates wear and tear on the sieve beds.
- Noise Levels: Portable units often have higher-pitched cooling fans compared to the muffled hum of a stationary unit.
- Safety: If your only device fails or the battery dies during a power outage, you have no backup.

Comparing Home vs. Portable: Which is Right for You?
| Feature | Home Oxygen Concentrator | Portable Oxygen Concentrator |
| Primary Use | Sleep and sedentary activities | Travel, shopping, and exercise |
| Flow Type | Continuous Flow | Pulse Dose (mostly) |
| Weight | Heavy (needs wheels) | Lightweight (backpack or strap) |
| Maintenance | Low (filter cleans) | Moderate (battery/sieve care) |
| Price (AUD) | $800 – $2,500 | $3,000 – $6,000+ |
Why “One Size Fits All” Often Costs More in the Long Run
Many Australians look at stationary oxygen units and POCs and think, “If I buy the most expensive portable, I don’t need the home unit.” From a senior strategist’s perspective, this is often a false economy. Here is why:
- Sieve Bed Replacement: POCs used 24/7 will require sieve bed replacements much sooner. These can cost hundreds of dollars.
- Electricity Efficiency: Stationary units are optimized for AC power. Running a POC off its charger constantly can degrade the battery’s lifespan.
- The “Sleep” Factor: Most medical professionals in Australia recommend continuous flow for sleeping to ensure blood oxygen saturation doesn’t drop during shallow breathing. Very few lightweight portables can provide this.
Step-by-Step: How to Choose Your Setup
Step 1: Consult Your Prescription
Your oxygen flow rate (LPM) is the ultimate gatekeeper. If you require 4LPM of continuous flow, almost all portable units are immediately disqualified as a primary source.
Step 2: Assess Your Activity Level
- Homebound: A high-quality stationary unit with a 15-metre hose is your best bet.
- Active/Social: You likely need a dual system (a home unit for night and a pulse-dose POC for day).
- Frequent Traveller: Invest in a POC that is FAA-approved and has long battery life.
Step 3: Evaluate Your Budget
While a single hybrid unit costs less than two separate machines initially, the cost of repairs and the shorter lifespan of the hybrid unit often balance the scales within 24 months.
Common Mistakes to Avoid
- Buying for Weight Only: Don’t buy the lightest unit if it doesn’t meet your oxygen needs.
- Ignoring the “Pulse Dose” Limitation: Many users find they cannot “trigger” the oxygen pulse when they are out of breath or sleeping.
- Buying Second-Hand without a Hour Meter Check: Always check how many hours the compressor has run before buying used.
FAQ: Frequently Asked Questions
1. Can I use my portable oxygen concentrator while I sleep?
Only if it has a “Continuous Flow” mode and your doctor has cleared it. Most POCs are “Pulse Dose,” which may not detect the shallow breathing patterns common during sleep.
2. Is a home oxygen concentrator louder than a portable one?
Actually, many modern stationary units are quieter (around 40-45 decibels) because they have more room for sound insulation. POCs can be noisier due to small, high-speed fans.
3. Do I need a regulator for a home concentrator?
No, home concentrators have built-in flow meters. Regulators are typically used for oxygen cylinders/tanks.
4. How long do the batteries last on a portable unit?
Depending on the setting, batteries usually last between 3 to 8 hours. Using a higher setting or continuous flow will drain the battery much faster.
5. Can I use a long hose with a portable oxygen concentrator?
It is not recommended. Portable units lack the pressure to push oxygen through long tubing. Most are limited to 2.1-metre (7ft) cannulas to ensure accurate pulse delivery.
Conclusion: The Best Solution for Australian Users
While the idea of all-in-one oxygen solutions is tempting, most users find that a “tag-team” approach is superior. Using a robust home oxygen concentrator for sleep and stationary time, paired with a lightweight portable oxygen concentrator for outings, provides the best reliability, therapy, and long-term cost savings.
Investing in the right equipment isn’t just about the price tag—it’s about ensuring your freedom of movement without compromising your clinical needs.
Internal Linking Suggestions:
- Anchor Text: “Guide to Medicare and Oxygen Equipment in Australia”
- Anchor Text: “How to maintain your oxygen concentrator filters”
- Anchor Text: “Top 5 portable oxygen concentrators for travel”
Authoritative External References:
- Lung Foundation Australia (Inquiry into respiratory equipment standards)
- Thoracic Society of Australia and New Zealand (TSANZ) Clinical Guidelines
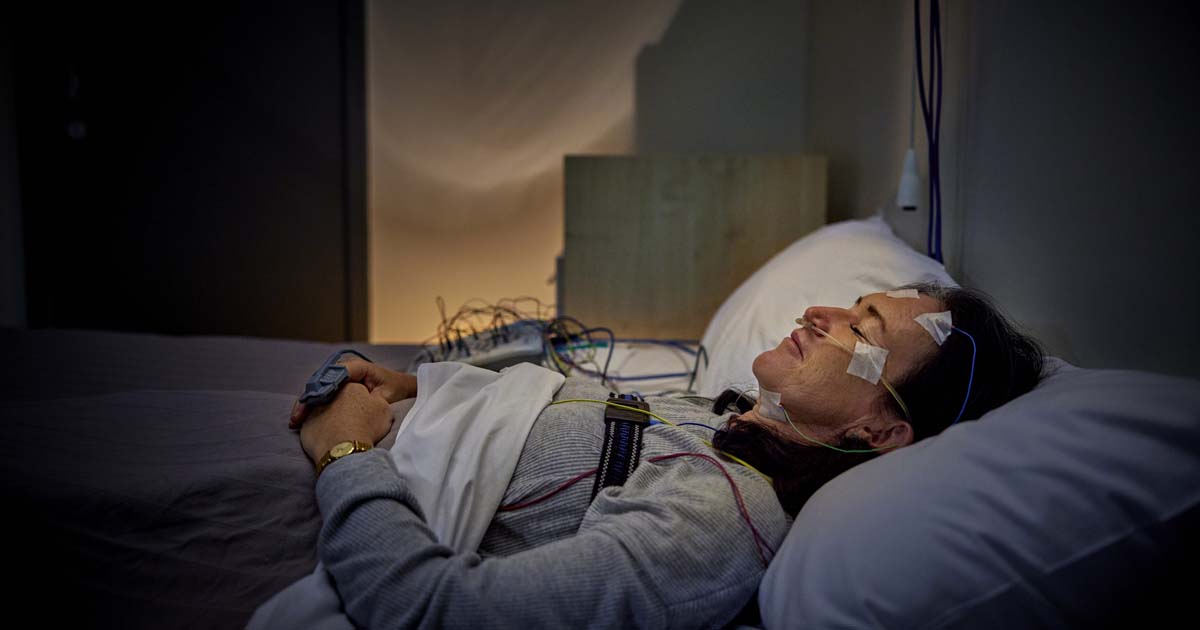
Understanding Your Sleep Study Report: What the Results Mean
This guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician.
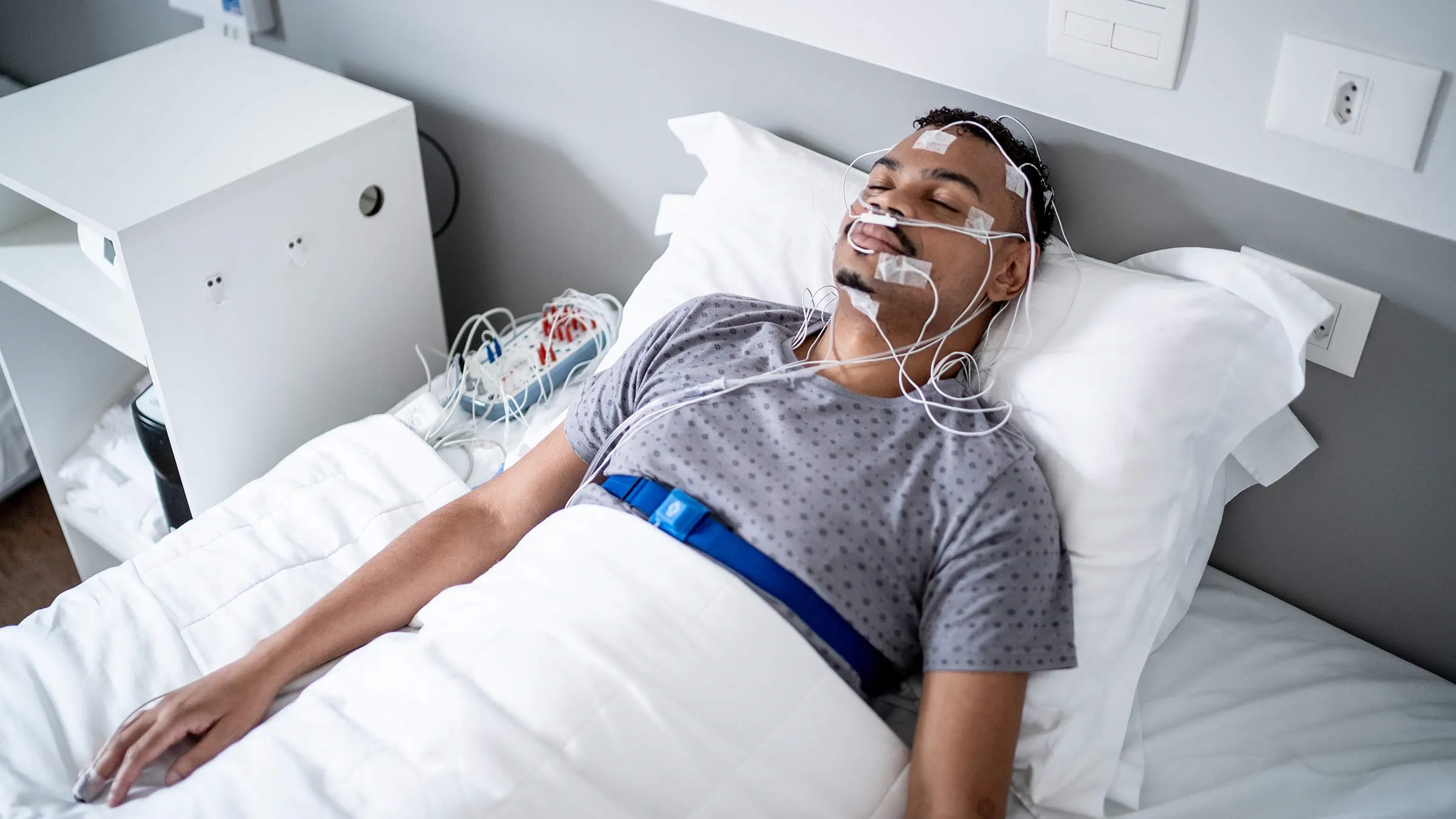
What is a sleep study report actually measuring?
A sleep study report explains how they sleep and how their body functions during sleep, with a particular focus on breathing and oxygen levels. Most reports combine data on brain activity, breathing effort, airflow, oxygen saturation, heart rate, and body movements to provide a comprehensive overview.
Depending on the type of test performed, the report may be based on a home sleep apnoea test (HSAT) or an in-lab polysomnography (PSG). In-lab reports are generally more detailed because they measure and classify actual sleep stages in addition to breathing patterns.
Which type of sleep study did they have, and why does it matter?
It matters because HSAT estimates sleep using recording time, while PSG measures sleep directly. That difference can change how indices are calculated and how confident a diagnosis is.
HSAT is commonly used when obstructive sleep apnoea is strongly suspected. PSG is often used when results are unclear, symptoms do not match HSAT findings, or when other conditions like parasomnias, narcolepsy, or periodic limb movement disorder are being considered.
What do “sleep stages” and “sleep architecture” mean in the report?
They describe how their sleep is divided across the night, usually into N1, N2, N3 (deep sleep), and REM sleep. A typical report shows time and percentage in each stage, plus a chart (hypnogram) of how stages change.
More fragmented sleep often shows as frequent awakenings, lots of light sleep (N1), and reduced deep or REM sleep. One abnormal night is not always meaningful, but patterns can explain symptoms like unrefreshing sleep.
What does “sleep efficiency” tell them?
Sleep efficiency is the percentage of time in bed (or recording time) spent asleep. Lower sleep efficiency usually means more time awake, more awakenings, or difficulty falling asleep.
Many labs flag low sleep efficiency because it can worsen daytime tiredness even when breathing indices are mild. It can also reduce REM sleep, which is important because breathing events sometimes cluster in REM.
What are apnoeas, hypopnoeas, and respiratory events?
They are breathing disturbances during sleep that can reduce airflow, oxygen, or cause arousals. An apnoea is typically a near-complete pause in airflow, while a hypopnoea is a partial reduction.
Reports may also include RERAs (respiratory effort-related arousals), which are subtler breathing events that fragment sleep. The exact definitions can vary slightly by lab rules, so the report’s scoring criteria matter.
What do AHI and RDI mean, and what is “normal”?
AHI (Apnoea–Hypopnoea Index) is the average number of apnoeas and hypopnoeas per hour of sleep (PSG) or per hour of recording (HSAT). RDI (Respiratory Disturbance Index) usually includes additional events like RERAs.
Many reports classify obstructive sleep apnoea severity roughly as: mild (5–14), moderate (15–29), severe (30+). “Normal” is often below 5, but symptoms, oxygen drops, and arousals still matter. Click here to get more about sleep apnea test Adelaide: 5 signs You should book one.
What is the difference between obstructive and central sleep apnoea in the results?
Obstructive events happen when the airway narrows or collapses while breathing effort continues. Central events happen when the brain temporarily reduces the drive to breathe, so effort drops too.
Most reports break events down into obstructive apnoeas, central apnoeas, mixed apnoeas, and hypopnoeas. A clinician looks at the pattern and proportion because treatment differs, especially if central events are prominent.
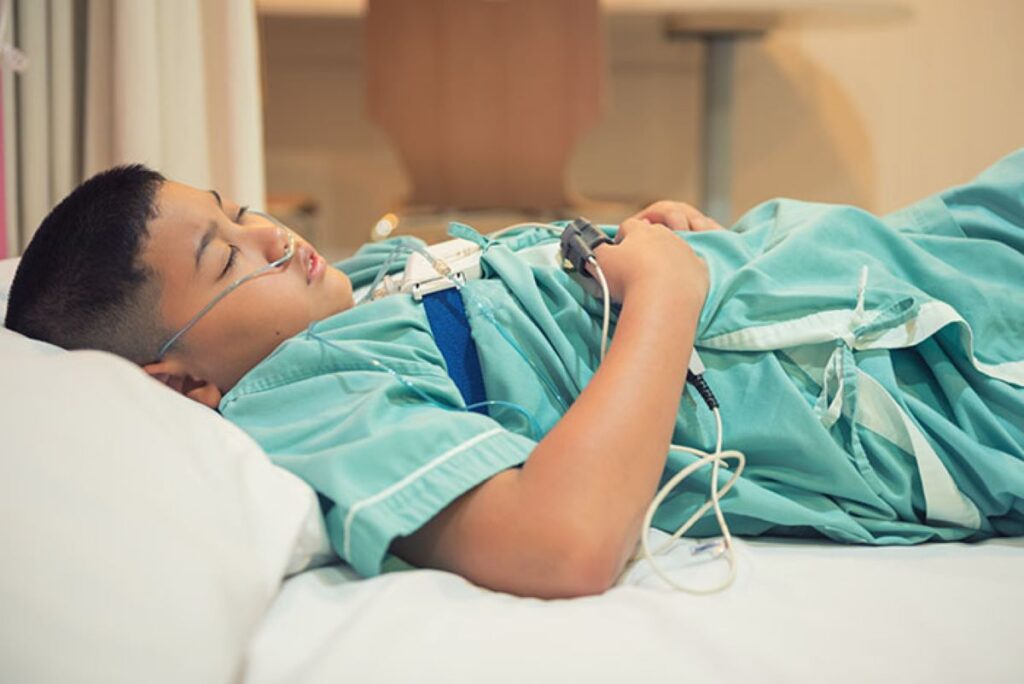
What does the oxygen section (SpO₂) mean for their health?
It shows how well oxygen levels stayed up during sleep and how often they dipped. Key values usually include baseline/mean SpO₂, the lowest SpO₂ (nadir), and time spent below thresholds such as 90%.
Brief dips can still be significant if they happen repeatedly. A low nadir or substantial time below 90% often pushes clinicians to treat more urgently, particularly in people with heart or lung conditions.
What is ODI, and why might it look different from AHI?
ODI (Oxygen Desaturation Index) counts how many oxygen drops occur per hour, often using a 3% or 4% drop rule. It can be lower than AHI if many breathing events cause arousals without major oxygen drops.
It can also be higher than AHI if oxygen drops occur for reasons other than scored apnoeas or hypopnoeas. Comparing AHI and ODI helps clinicians see whether events are mainly desaturation-driven or arousal-driven.
Other Resources : Understanding the sleep cycle
What do arousals and awakenings mean, and why do they matter?
Arousals are brief disruptions in sleep that can prevent deep, restorative sleep, even if they do not fully wake them. Reports may list an arousal index (arousals per hour) and sometimes link arousals to breathing, movement, or spontaneous causes.
High arousal rates often explain fatigue, headaches, poor concentration, and mood changes. Someone can have a borderline AHI but still feel awful if sleep is repeatedly fragmented.
What do heart rate and rhythm findings usually indicate?
Most sleep studies track heart rate and may note irregular rhythms. Many reports simply show average and range, but some include comments on ectopic beats or suspected atrial fibrillation patterns.
An elevated heart rate during clusters of breathing events can support the idea that apnoea is stressing the cardiovascular system. If the report flags rhythm concerns, it usually prompts follow-up rather than providing a definitive cardiac diagnosis.
What do limb movements (PLMS) mean in the report?
PLMS (Periodic Limb Movements in Sleep) are repetitive leg movements that can fragment sleep. Reports may show a PLM index and a PLM arousal index, which is often the more important number.
PLMS can occur on their own or alongside conditions like restless legs syndrome. Treatment decisions typically depend on symptoms, sleep disruption, iron status, and whether breathing events are also present.
What is body position data, and why does it change the interpretation?
Position data shows whether events are worse on the back (supine) versus side or front. Many people have “positional” obstructive sleep apnoea, where AHI is significantly higher when supine.
If the report shows a strong positional pattern, clinicians may discuss side-sleeping strategies, positional devices, or targeted therapy. It also helps explain why symptoms can vary night to night.
What does REM-related sleep apnoea mean?
It means breathing events cluster mainly during REM sleep. This can happen even when the overall AHI looks mild because REM can make the airway more collapsible.
REM-related apnoea may still cause significant oxygen dips and vivid sleep disruption. It is especially relevant if the study captured little REM, because limited REM can underestimate severity.
How do they know if the results match the symptoms?
They compare the numbers with the clinical picture: snoring, witnessed pauses, choking awakenings, daytime sleepiness, morning headaches, and concentration problems. They also consider comorbidities like hypertension, diabetes, reflux, or depression.
A report can look “mild” but still justify treatment if symptoms and oxygen findings are significant. Conversely, some people with higher AHI may report fewer symptoms, and treatment choices may prioritise long-term risk reduction.

What do common recommendations (CPAP, APAP, oral appliance) mean?
They are options to keep the airway open and improve sleep quality. CPAP provides fixed pressure, while APAP adjusts within a range; reports may recommend pressure settings or a trial.
Oral appliances reposition the jaw and can help in mild to moderate obstructive sleep apnoea, especially if they cannot tolerate CPAP. Recommendations often also include weight management (if relevant), avoiding alcohol near bedtime, and treating nasal obstruction.
What should they ask at the follow-up appointment?
They should ask which result drove the diagnosis, whether the test likely underestimated severity, and what success looks like in their case. They can also ask how to measure improvement: symptoms, device data, repeat testing, or blood pressure changes.
Helpful questions include: which events were obstructive versus central, whether oxygen dips were concerning, whether sleep was fragmented by arousals, and whether position or REM made it worse. The goal is a plan that fits both the numbers and how they feel.
FAQs (Frequently Asked Questions)
What does a sleep study report measure and why is it important?
A sleep study report measures how a person sleeps and how their body behaves during sleep, focusing on breathing, oxygen levels, brain activity, heart rate, and movement. This comprehensive data helps clinicians understand sleep quality and diagnose conditions like obstructive sleep apnoea or other sleep disorders.
How do home sleep apnoea tests (HSAT) differ from in-lab polysomnography (PSG) in sleep studies?
HSAT estimates sleep based on recording time and is typically used when obstructive sleep apnoea is strongly suspected. PSG measures actual sleep stages directly in a lab setting, providing more detailed information useful for unclear cases or when diagnosing complex conditions like parasomnias or narcolepsy.
What are sleep stages and how do they affect the interpretation of a sleep study report?
Sleep stages refer to the division of sleep into N1, N2, N3 (deep sleep), and REM phases. Sleep architecture shows the time spent in each …
Read MoreSleep Apnea Test Adelaide: 5 Signs You Should Book One
If they live in Adelaide and recognise the signs below, booking a sleep apnoea test is often the fastest way to get clarity and start feeling better.
What exactly is sleep apnoea, and why does testing matter?
A sleep apnea test Adelaide service is used to diagnose sleep apnoea, a sleep-related breathing disorder where airflow repeatedly reduces or stops during the night. These breathing pauses can disrupt sleep cycles and lower oxygen levels, often without the person being fully aware.
Testing is important because symptoms can overlap with stress, insomnia, and general lifestyle fatigue. A properly conducted sleep study can confirm whether sleep apnoea is present, determine its severity, and guide the most appropriate treatment approach.
Is loud, frequent snoring a sign they should book a sleep apnoea test in Adelaide?
Yes, especially when snoring is loud, nightly, and has been worsening over time. Snoring can happen without sleep apnoea, but persistent snoring is one of the most common red flags.
If others report snoring plus choking, snorting, or gasping sounds, it becomes more concerning. Those noises can reflect the airway repeatedly narrowing and reopening, which is typical in obstructive sleep apnoea.
Have they been told they stop breathing or gasp during sleep?
Yes, this is one of the clearest reasons to book a test. Many people with sleep apnoea do not remember waking, but a partner may notice repeated pauses followed by a gasp.
If they sleep alone, clues can include waking suddenly with a racing heart, feeling out of breath, or experiencing unexplained night-time panic. A sleep study can identify how often these events occur and whether oxygen drops are involved.
Are they waking up tired even after a full night in bed?
Yes, unrefreshing sleep is a common sign. Someone may spend 7–9 hours in bed and still wake feeling as if they barely slept.
That often happens because sleep apnoea causes repeated micro-arousals that stop them reaching or staying in deeper sleep stages. Over time, the result can be daytime sleepiness, poor concentration, irritability, and a higher risk of nodding off during quiet activities.
Do they have morning headaches, dry mouth, or a sore throat?
Yes, especially when it happens regularly. Morning headaches can be linked to changes in oxygen and carbon dioxide levels overnight, as well as disrupted sleep.
Dry mouth and a sore throat can suggest mouth breathing, which is common when the airway is partially blocked through the nose or throat. While these symptoms can have other causes, recurring patterns are a good reason to investigate with a sleep apnoea test. You may like to visit https://www.health.vic.gov.au/statewide-referral-criteria/sleep-disordered-breathing to get more about sleep disordered breathing.
Are they dealing with high blood pressure, heart symptoms, or type 2 diabetes risk?
Often, yes, they should consider testing. Sleep apnoea is associated with higher cardiovascular strain because the body repeatedly reacts to oxygen drops and disrupted sleep.
If they have high blood pressure that is hard to control, irregular heart rhythms, or other heart concerns, clinicians often want sleep apnoea ruled in or out. The same goes for people with insulin resistance or type 2 diabetes risk, where sleep quality can play a role in metabolic health. Read more about understanding your sleep study report: what the results mean.
What should they expect when booking a sleep apnoea test in Adelaide?
Most people are offered either a home sleep study or an in-clinic overnight study. Home studies are convenient and can be a strong first step for suspected obstructive sleep apnoea.
An in-clinic study is more comprehensive and may be recommended when symptoms are complex, another sleep disorder is suspected, or earlier results were unclear. After the test, results typically include an index of breathing events and oxygen changes, which guides next steps.
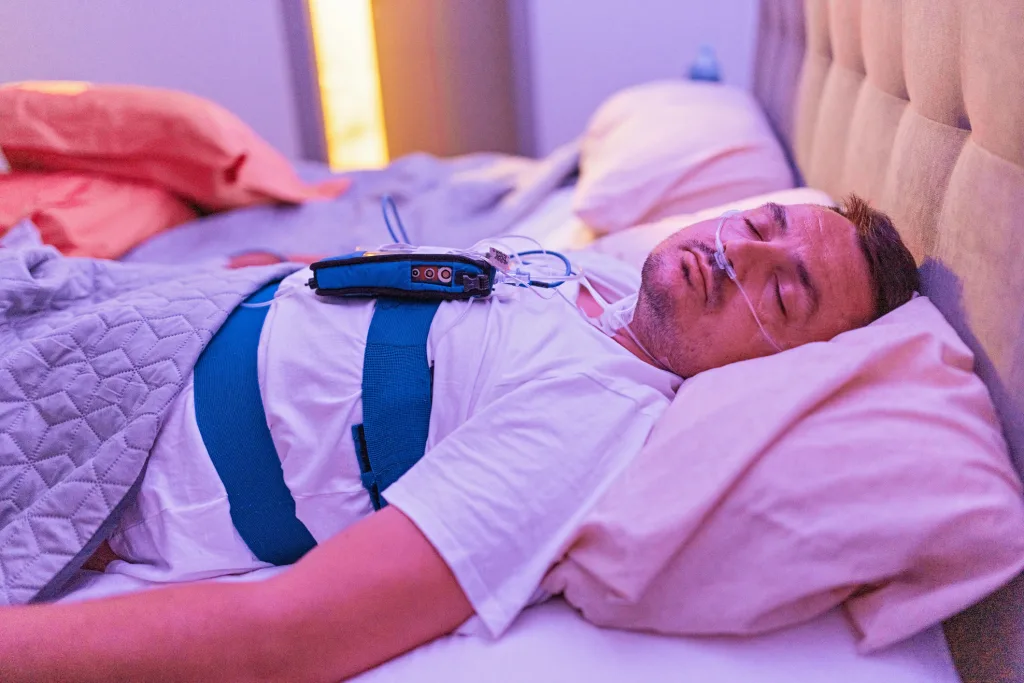
If they recognise one or more signs, what should they do next?
They should book an appointment with a GP or a sleep clinic to discuss symptoms and testing options. Bringing a short symptom list helps, including snoring reports, observed breathing pauses, daytime sleepiness, and any relevant medical history.
The goal is simple: confirm what is happening during sleep, then choose a plan that improves breathing and restores proper rest. For many, the difference after proper diagnosis and treatment is not subtle.
FAQs (Frequently Asked Questions)
What is sleep apnoea and why is it important to get tested?
Sleep apnoea is a sleep-related breathing disorder where airflow reduces or stops repeatedly during the night, causing fragmented sleep and drops in oxygen levels. Testing is important because its symptoms can overlap with stress, insomnia, and fatigue. A proper sleep study confirms if sleep apnoea is present, its severity, and helps determine the best treatment.
Is loud and frequent snoring a sign that I should book a sleep apnoea test in Adelaide?
Yes, especially if your snoring is loud, occurs nightly, and has worsened over time. Persistent snoring is a common red flag for sleep apnoea. If others report snoring accompanied by choking, snorting, or gasping sounds, it becomes even more concerning as these reflect airway narrowing typical in obstructive sleep apnoea.
What does it mean if I stop breathing or gasp during sleep?
Stopping breathing or gasping during sleep are clear signs of potential sleep apnoea. Many people don’t remember waking up but partners may notice repeated pauses followed by gasps. If you sleep alone, sudden waking with a racing heart or feeling out of breath can be clues. A sleep study can determine how often these events occur and if oxygen levels drop.
Why do I wake up tired even after a full night’s sleep?
Waking up unrefreshed despite spending 7–9 hours in bed can indicate sleep apnoea. The condition causes repeated micro-arousals that prevent reaching or maintaining deep sleep stages. Over time, this leads to daytime sleepiness, poor concentration, irritability, and increased risk of nodding off during quiet activities.
Are morning headaches, dry mouth, or sore throat signs of sleep apnoea?
Yes, especially if these symptoms happen regularly. Morning headaches may be linked to overnight changes in oxygen and carbon dioxide levels along with disrupted sleep. Dry mouth and sore throat suggest mouth breathing due to partial airway blockage in the nose or throat. Recurring patterns warrant investigation through a sleep apnoea test.
How does sleep apnoea relate to high blood pressure and other health risks?
Sleep apnoea increases cardiovascular strain because the body reacts repeatedly to oxygen drops and disrupted sleep. If you have high blood pressure that’s difficult to control, irregular heart rhythms, or concerns about type 2 diabetes risk, testing for sleep apnoea is advised as it can impact metabolic health and heart function.
… Read MoreUltimate Guide to Choosing an Oxygen Concentrator in Australia (2026)
ntroduction to Modern Oxygen Therapy
For many Australians living with chronic respiratory conditions, maintaining an active lifestyle in cities like Sydney requires more than just medical advice—it requires the right technology. An oxygen concentrator is a life-changing medical device that provides a continuous or pulse-dose supply of oxygen by filtering ambient air. Unlike traditional tanks that require refilling, these devices offer independence and peace of mind.
Whether you are navigating the hilly streets of Surry Hills or planning a trip across the Blue Mountains, understanding how an oxygen concentrator works is the first step toward reclaiming your mobility. This guide explores the technical nuances, clinical benefits, and the specific advantages of industry leaders like the Zen-O portable oxygen concentrator.
What is an Oxygen Concentrator?
An oxygen concentrator is an electrically powered medical device designed to concentrate oxygen from the surrounding air. The air we breathe is approximately 21% oxygen and 78% nitrogen. The concentrator pulls this air in, filters out the nitrogen, and delivers medical-grade oxygen (usually 90%–95% purity) to the user via a nasal cannula or mask.
How the Technology Works
The core of the device lies in its “molecular sieve” technology. Using Pressure Swing Adsorption (PSA), the device cycles air through two cylinders filled with zeolite pellets.
- Intake: Ambient air is compressed into the first cylinder.
- Adsorption: The zeolite traps nitrogen molecules while allowing oxygen to pass through.
- Delivery: The purified oxygen is collected in a reservoir and delivered to the patient.
- Purge: The system releases the trapped nitrogen back into the atmosphere and switches to the second cylinder to ensure a continuous flow.
Stationary vs. Portable Oxygen Concentrators
In the Australian market, devices are generally categorized into two types based on their intended use and flow capabilities.
| Feature | Stationary Concentrator | Portable Oxygen Concentrator (POC) |
| Weight | 14kg – 25kg | 2kg – 5kg |
| Power Source | AC Wall Outlet | Internal Battery, AC, or DC (Car) |
| Flow Type | Continuous Flow | Pulse Dose (mostly) |
| Ideal For | Sleep and home use | Travel, shopping, and exercise |
| Example | High-capacity home units | Zen-O portable oxygen concentrator |
Spotlight on the Zen-O Portable Oxygen Concentrator
When discussing mobility, the Zen-O portable oxygen concentrator stands out as a versatile “all-rounder” for Sydney residents. Manufactured by GCE Healthcare, it is specifically designed for patients who require a higher oxygen output but do not want to be confined to their homes.
Key Benefits of the Zen-O
- Dual Mode Delivery: Unlike many smaller units, the Zen-O can provide both pulse dose (triggered by inhalation) and continuous flow (up to 2 liters per minute).
- Field-Replaceable Sieve Beds: In the humid conditions of coastal NSW, sieve beds can wear down. The Zen-O allows users or providers to swap these parts easily without sending the whole unit for repair.
- Rugged Design: Built to handle the vibrations of car travel and frequent movement.
- Rate Response Therapy: The device automatically increases the oxygen dose if it detects the user is walking or exerting themselves.
Clinical Benefits and Outcomes
Using a high-quality oxygen concentrator as prescribed by an Australian respiratory specialist can lead to significant health improvements:
- Increased Survival: Long-term oxygen therapy (LTOT) is proven to extend life in patients with severe COPD.
- Enhanced Exercise Tolerance: Supplemental oxygen reduces breathlessness during physical activity, allowing for better muscle maintenance.
- Improved Cognitive Function: Proper oxygenation prevents the “brain fog” often associated with hypoxemia.
- Better Sleep Quality: Consistent oxygen levels at night prevent frequent awakenings and heart strain.
Step-by-Step: Selecting the Right Device in Sydney
Choosing a device involves more than just comparing prices. Follow this framework to ensure the best fit for your medical needs:
1. Consult Your Pulse Oximetry Data

Your specialist will determine your “liters per minute” (LPM) requirement. Ensure the device you choose can exceed your highest required flow rate to allow for future needs.
2. Evaluate Your Lifestyle
Do you spend most of your time at home, or do you enjoy walks along the Bondi to Coogee coastal path? If you are active, a lightweight POC like the Zen-O portable oxygen concentrator is essential.
3. Check Battery Life and Charging
In Australia, travel distances can be long. Look for devices with “Extended Battery” options and those that can charge via a 12V DC outlet (cigarette lighter) in your vehicle.
4. Noise Levels
If you intend to use the device in quiet environments like the State Library or at the cinema, look for a unit with a decibel rating under 45dB.
Best Practices for Maintenance and Safety
To ensure your oxygen concentrator remains efficient and fast-tracks your health goals, follow these expert tips:
- Clean the Particle Filter: Wash the external dust filter weekly with warm soapy water and air-dry it completely.
- Avoid Smoking and Open Flames: Oxygen is an accelerant. Maintain a distance of at least 3 meters from gas stoves or cigarettes.
- Keep the Unit Well-Ventilated: Never place your concentrator in a closet or against heavy curtains, as it needs fresh air to function and cool its internal motor.
- Use Distilled Water: If your stationary unit uses a humidifier bottle, only use distilled water to prevent mineral buildup.
Common Mistakes to Avoid
- Buying Without a Prescription: Oxygen is a drug. Using too much can lead to oxygen toxicity; using too little can cause organ damage.
- Ignoring Altitude Settings: If you are flying out of Sydney Kingsford Smith Airport, ensure your POC is FAA-approved and that you have 150% of the flight duration in battery life.
- Neglecting the Cannula: Replace your nasal cannula every 2–4 weeks to prevent bacterial growth and ensure optimal flow.
Internal & External Resource Suggestions
- Internal Link Suggestion: “Comparing Portable Oxygen Concentrator Battery Life” (Anchor: portable oxygen concentrator battery)
- Internal Link Suggestion: “Top 5 Tips for Traveling with Medical Oxygen” (Anchor: traveling with oxygen)
- External Reference: Refer to the Lung Foundation Australia for clinical guidelines on COPD management.
- External Reference: Consult the Therapeutic Goods Administration (TGA) for medical device safety standards in Australia.
Frequently Asked Questions (FAQ)
What is the lifespan of an oxygen concentrator?
Most high-quality units are designed to last between 5 and 7 years, or approximately 15,000 to 20,000 hours of use, provided they are serviced regularly.
Can I use a portable oxygen concentrator at night?
Yes, but only if the device has a “Continuous Flow” mode or a highly sensitive pulse trigger that detects shallow breathing during sleep. The Zen-O is a popular choice for this.
Is an oxygen concentrator better than a tank?
A concentrator is generally more convenient because it never runs out of oxygen as long as it has power. However, tanks do not require electricity and are silent.
How much electricity does a stationary unit use?
On average, a home oxygen concentrator uses about the same amount of power as a standard refrigerator or a desktop computer.
Are oxygen concentrators loud?
Stationary units produce a “humming” sound. Modern portable units are much quieter, often compared to the sound of a small electric fan.
Conclusion: Investing in Your Respiratory Freedom
Choosing the right oxygen concentrator is a significant decision that impacts your health, mobility, and overall quality of life. By focusing on reliable brands like the Zen-O portable oxygen concentrator and adhering to a strict maintenance schedule, residents in Sydney and across Australia can continue to engage in the activities they love.
Always ensure your device is sourced from a reputable Australian supplier that offers local warranty support and servicing to avoid long downtimes.
… Read MoreThe Best CPAP Mask Options for New Users and What Makes Them Comfortable
Sleep apnea disrupts breathing during sleep, causing repeated pauses that prevent restful sleep and strain the cardiovascular system. CPAP therapy delivers continuous pressurized air through a mask, keeping airways open throughout the night and enabling uninterrupted breathing.
The mask serves as the critical connection point between the machine and the user. New CPAP users often struggle with therapy because they haven’t found the right mask for their needs. A poorly fitting or uncomfortable mask leads to air leaks, skin irritation, and restless nights—problems that quickly discourage people from continuing treatment.
Comfort directly determines whether someone will stick with CPAP therapy. Studies show that users who find their masks comfortable are significantly more likely to use their devices consistently. The right mask should feel secure without causing pressure points, match individual breathing patterns, and accommodate personal sleep habits.
Finding the best CPAP mask options for new users requires understanding how different designs work with various face shapes, sleeping positions, and breathing styles. The journey to successful sleep apnea therapy begins with selecting a mask that feels natural rather than intrusive. When new CPAP users prioritize CPAP comfort from the start, they set themselves up for better sleep quality and improved long-term health outcomes.
What Are the Main Types of CPAP Masks Available for New Users?
New users can choose from four primary CPAP mask types, each designed to address specific breathing patterns and comfort preferences. Understanding these options helps match the right mask to individual needs from the start.
1. Nasal Pillow Masks
Nasal pillow masks feature small, soft cushions that seal directly at the nostrils without covering the nose. This lightweight design minimizes facial contact, making them ideal for people who feel claustrophobic, wear glasses to bed, or have facial hair that interferes with larger mask seals. Side sleepers particularly appreciate how these masks avoid bulk that might press into pillows.
2. Nasal Masks
Nasal masks cover the entire nose with a triangular cushion held in place by adjustable headgear. These work best for nose breathers who need higher pressure settings, as the broader seal distributes air pressure more evenly across the nasal area. Active sleepers benefit from the secure fit that stays in place during movement.
3. Full-Face Masks
Full-face masks (oronasal masks) seal around both the nose and mouth, delivering therapy regardless of whether you breathe through your nose, mouth, or both. Mouth breathers, people with chronic nasal congestion, and those experiencing air leaks with smaller masks find these most effective, despite the larger profile.
4. Hybrid Masks
Hybrid masks combine nasal pillow technology with mouth coverage, offering a middle ground between full-face bulk and nasal pillow minimalism. This design suits mouth breathers seeking less facial coverage than traditional full-face options provide.
How Do Breathing Habits Influence the Choice of CPAP Mask?
Your natural breathing pattern during sleep directly determines which CPAP mask will work best for you.
Nose Breathers
Nose breathers can comfortably use nasal pillow masks or standard nasal masks since they naturally keep their mouths closed throughout the night, allowing the pressurized air to flow exclusively through nasal passages.
Mouth Breathers
Mouth breathers face different requirements entirely. If you breathe through your mouth during sleep—whether habitually or due to nasal congestion, allergies, or deviated septum—nasal-only masks will fail to deliver therapy effectively. Air escapes through the open mouth, creating mouth leaks that reduce pressure levels and compromise treatment quality.
The Importance of Full-Face Masks
Full-face masks become essential for mouth breathers because they seal around both the nose and mouth, ensuring pressurized air reaches your airway regardless of breathing pattern. Hybrid masks offer a lighter alternative while still accommodating mouth breathing, combining nasal pillows with a mouth cushion for complete coverage without the bulk.
The Impact of Mouth Leaks
The impact of mouth leaks extends beyond comfort concerns:
- Reduced therapy effectiveness as prescribed pressure levels drop
- Dry mouth and throat irritation from constant air exposure
- Disrupted sleep quality from mask noise and air turbulence
- Lower treatment compliance due to discomfort
Considerations for Chronic Nasal Congestion
Users experiencing chronic nasal congestion should consider full-face or hybrid options even if they typically breathe through their nose, as nighttime stuffiness can force mouth breathing and create unexpected leaks.
How Do Sleeping Positions Affect CPAP Mask Comfort and Fit?
Your preferred sleeping position directly determines which mask design will stay secure throughout the night. Side sleepers typically experience the most challenges with bulkier masks that press into pillows, causing air leaks and discomfort.
CPAP Masks for Side Sleepers
Side sleepers benefit most from nasal pillow masks because their low-profile design sits below the pillow line. These minimal masks eliminate the bulk that pushes against bedding, preventing the seal disruption that larger masks experience. The compact footprint allows natural head positioning without compromising therapy pressure delivery. However, side sleeping can also create specific pressure points that affect long-term comfort, requiring cushions that distribute pressure evenly.
CPAP Masks for Back Sleepers
Back sleepers have more flexibility in mask selection since gravity naturally helps maintain seal contact. Full-face masks and traditional nasal masks work well for this position, though securing proper headgear tension remains important. The stable position reduces shifting that could break the seal, making these sleepers ideal candidates for masks with broader cushion contact.
CPAP Masks for Stomach Sleepers
Stomach sleepers face similar challenges to side sleepers, needing ultra-minimal designs that won’t dislodge during movement. These individuals often require specific adjustments to their CPAP therapy to accommodate their unique sleeping posture.
The Impact of Sleep Position on Mask Stability
Mask stability depends on how your sleep position interacts with headgear straps. Active sleepers who change positions frequently need adjustable straps that maintain consistent tension across different angles, preventing both overtightening and seal breaks during natural nighttime movement.
For those experiencing discomfort due to shoulder pain while trying to adjust their sleeping position for better CPAP mask fit, exploring strategies on how to sleep with shoulder pain might provide some relief. Additionally, understanding the best sleeping position for sleep apnea can further enhance the effectiveness of CPAP therapy by promoting better airflow and reducing symptoms during sleep.
Other Resources : Management of obstructive sleep apnoea in primary care

How Do Facial Features and Accessories Impact Mask Selection?
1. Facial Hair: Choosing the Right CPAP Mask
For individuals with facial hair, selecting the appropriate CPAP mask becomes crucial. Beards and mustaches can create gaps between the mask cushion and the skin, compromisiasdng the seal necessary for effective therapy. Men with facial hair often discover that nasal pillow masks are the most suitable option since they provide a direct seal at the nostrils instead of across the upper lip or cheeks where hair grows. This design effectively avoids the common leak points that frustrate users of traditional nasal or full-face masks.
2. Glasses Wearers: Finding Compatible CPAP Masks
Glasses wearers have specific requirements when it comes to choosing CPAP masks. Designs that minimize contact with the face and strategically place straps are beneficial in this case. Masks featuring top-of-head harnessing or those that avoid the bridge of the nose prevent interference with eyeglass frames during activities such as bedtime reading or watching TV. Nasal pillow masks excel in this aspect by leaving the face mostly unobstructed, allowing users to comfortably wear glasses before removing them for sleep.
3. Addressing Claustrophobia: Masks for Comfort
Claustrophobia concerns can be alleviated by opting for masks that provide less coverage on the face and maintain an open field of vision. Users who feel confined by traditional full-face masks tend to respond better to:
- Nasal pillow designs that only make contact with the nostrils
- Lightweight frames that reduce the sensation of wearing equipment
- Clear sight lines that prevent a “closed-in” feeling
4. Adapting to Face Shape Variations
Variations in face shape, such as narrow or wide bridges, prominent cheekbones, or recessed features, necessitate cushion designs that can adapt to individual contours. Masks equipped with flexible silicone cushions and multiple sizing options are capable of accommodating these differences, thereby preventing pressure sores and ensuring a consistent seal throughout the night.
Why Is Proper Sizing and Fit Crucial for Comfort in CPAP Masks?
Does an improperly sized mask affect therapy success?
Yes—incorrect CPAP mask fit leads to air leaks that compromise therapy pressure, reducing treatment effectiveness and causing sleep disruptions. Leaks also create irritating noise and dry out eyes or skin from escaping air streams. A properly sized mask maintains consistent seal contact throughout the night, delivering prescribed pressure levels without interruption.
How do adjustable components improve individual comfort?
Adjustable straps CPAP systems feature multiple adjustment points on headgear, allowing users to customize tension distribution across their head and face. These straps prevent the mask from being too loose (causing leaks) or too tight (creating painful pressure marks). Cushions come in various sizes—small, medium, large, and sometimes wide options—to accommodate different facial dimensions. Users often need to try multiple cushion sizes even within the same mask model to find their optimal fit.
What cushion materials affect skin comfort during
… Read MoreOxygen Machine for Home Use: A Complete Guide for First-Time Buyers
What Is an Oxygen Machine and How Does It Work?
An oxygen machine for home use, commonly known as an oxygen concentrator, is a medical device that delivers concentrated oxygen to individuals with respiratory conditions. These respiratory therapy devices extract oxygen from the surrounding air and provide it at higher concentrations than what’s naturally available, typically delivering medical-grade oxygen at 90-95% purity.
The primary function centers on supporting patients whose lungs cannot adequately absorb oxygen from normal air. Conditions like chronic obstructive pulmonary disease (COPD), emphysema, severe asthma, and pulmonary fibrosis often require supplemental oxygen to maintain healthy blood oxygen saturation levels.
The Oxygen Extraction Process
The An Oxygen Machine for Home Use operates using a sophisticated yet reliable technology known as Pressure Swing Adsorption (PSA). This process converts normal room air—which contains approximately 21% oxygen and 78% nitrogen—into concentrated oxygen suitable for medical therapy.
Here’s how an Oxygen Machine for Home Use extracts oxygen:
• Air intake: The machine draws ambient air through an inlet filter
• Compression: An internal compressor pressurizes the air
• Nitrogen separation: Compressed air passes through zeolite molecular sieves that capture nitrogen molecules
• Oxygen collection: The remaining oxygen-rich gas is collected in a reservoir
• Delivery: Concentrated oxygen is delivered to the patient via tubing connected to a nasal cannula or mask
The zeolite material acts as a highly selective filter, allowing oxygen molecules to pass while trapping nitrogen. Most Oxygen Machines for Home Use utilize dual sieve beds that alternate between oxygen collection and nitrogen release, ensuring a continuous, uninterrupted oxygen supply.
Supporting Blood Oxygen Levels
Medical-grade oxygen plays a critical role in maintaining adequate blood oxygen saturation for respiratory patients. Healthy individuals typically maintain oxygen saturation levels between 95-100%, but those with compromised lung function often drop below this range, leading to hypoxemia.
When blood oxygen levels fall too low, the body’s organs and tissues don’t receive sufficient oxygen to function properly. This oxygen deprivation can cause:
- Shortness of breath and rapid breathing
- Increased heart rate as the body compensates
- Fatigue and confusion
- Bluish discoloration of lips or fingertips (cyanosis)
Why Is It Important to Buy From a Reputable Retailer?
Reputable oxygen concentrator sellers protect your health and legal standing. Trusted retailers require a valid prescription from your healthcare provider before completing any sale, ensuring the device matches your specific medical needs and oxygen flow requirements.
Legal Requirements You Cannot Ignore
Medical-grade oxygen legality demands proper documentation. Oxygen qualifies as a controlled substance under federal regulations, as outlined in this legal document. Purchasing without a prescription violates these laws and exposes buyers to legal consequences. Legitimate sellers verify prescriptions because they understand these requirements protect both parties.
Health Risks of Substandard Equipment
Unverified retailers often sell devices that:
- Fail to maintain consistent oxygen purity levels
- Lack proper safety mechanisms against equipment failure
- Come without manufacturer warranties or support
- May contain counterfeit or expired components
These deficiencies create dangerous situations for patients depending on supplemental oxygen therapy. A malfunctioning concentrator can lead to hypoxemia, where blood oxygen drops to critical levels.
The Prescription Requirement Serves Multiple Purposes
Your doctor’s prescription specifies the exact oxygen flow rate and usage schedule your condition requires. This information guides retailers in recommending appropriate equipment capacity. The prescription also establishes medical necessity for insurance claims and creates a paper trail for warranty service or equipment recalls.
Authorized medical equipment suppliers maintain relationships with manufacturers, providing access to technical support, replacement parts, and service networks. These connections prove invaluable when troubleshooting issues or maintaining your device over its lifespan.
What Are the Differences Between New, Used, and Refurbished Oxygen Machines?
New Oxygen Concentrators
New oxygen concentrators arrive untouched by previous users and typically include manufacturer warranties ranging from one to five years. These machines deliver maximum longevity with minimal repair needs during their early years of operation. Buyers receive the latest technology features, updated safety mechanisms, and full documentation. The higher upfront cost translates to peace of mind through guaranteed performance and comprehensive support from manufacturers.
Used Oxygen Concentrators
Used oxygen concentrators present a middle ground between premium pricing and budget constraints. These units have served previous owners but undergo thorough testing to verify full functionality before resale. Reputable sellers inspect critical components like flow rates, oxygen purity levels, and alarm systems. The reduced price point makes oxygen therapy accessible to patients with limited financial resources, though buyers should expect shorter remaining lifespans compared to new models. Warranty coverage varies significantly—some used units carry limited seller guarantees while others offer no protection against future malfunctions.
Refurbished Oxygen Machines
Refurbished oxygen machines receive professional restoration through replacement of worn components. Technicians commonly replace sieve beds, filters, and other parts that degrade with extended use. This process restores the concentrator to near-original performance standards at a fraction of new equipment costs. Quality refurbishment includes recalibration, cleaning, and comprehensive testing protocols as per the FDA regulatory requirements. Buyers gain access to reliable equipment while saving 30-50% compared to new purchases. Certified refurbished units often include warranties, though coverage periods typically span shorter durations than new machine guarantees.
The choice between new vs used oxygen concentrators depends on individual circumstances:
- Budget availability: New units require larger initial investments
- Expected usage duration: Long-term needs justify new equipment costs
- Risk tolerance: Used machines carry higher uncertainty about future repairs
- Warranty preferences: New concentrators provide strongest protection
Renting Oxygen Concentrators
Renting oxygen concentrators serves patients requiring temporary oxygen support. Short-term medical situations like post-surgical recovery or acute respiratory infections benefit from rental arrangements. Monthly rental fees eliminate large upfront expenses, though extended rental periods eventually exceed purchase costs. Rental companies handle maintenance and repairs, removing technical responsibilities from patients. This cost-effective option works best for needs lasting weeks to a few months rather than permanent oxygen therapy requirements.
Whether you opt for a new or used model, it’s essential to understand the specifics of your situation and the available options including oxygen equipment accessories which can further enhance your treatment experience.
How Can Package Deals Benefit First-Time Buyers?
Package deals combine your oxygen concentrator with essential oxygen concentrator accessories in a single purchase, typically offering better value than buying each item separately. Most bundles include practical items like carrying cases for portability, extra batteries for extended use away from power outlets, and additional charging cables for convenience.
The cost savings on accessories through bundled purchases can be substantial. When retailers package these items together, they often reduce the total price by 15-30% compared to individual purchases. A carrying case alone might cost $50-100 separately, while batteries can run $150-300 each, and spare charging cables typically retail for $30-50. Buying these as a package deal can save first-time buyers $100-200 or more.
Common package inclusions:
- Protective carrying cases or backpacks designed for specific concentrator models
- Spare rechargeable batteries (especially valuable for portable units)
- Extra charging cables and AC/DC power adapters
- Cannulas and tubing for oxygen delivery
- Filters and maintenance supplies
- Travel accessories like car chargers
Shipping costs represent another advantage of package deals. Rather than placing multiple orders and paying separate shipping fees for each accessory, bundled purchases arrive in one shipment. This consolidation saves money and reduces the waiting time to receive all necessary equipment.
Package deals also eliminate the guesswork about compatibility. Retailers curate accessories specifically matched to your concentrator model, ensuring proper fit and function. This removes the risk of ordering incompatible parts and the hassle of returns or exchanges. For first-time buyers unfamiliar with oxygen concentrator accessories, this pre-selected approach provides peace of mind while setting up home oxygen therapy.
Moreover, it’s worth noting that certain medical guidelines suggest specific combinations of equipment and accessories that work best together. By opting for a package deal, first-time buyers can ensure they are following these recommendations while also saving money and time.

When Should Buyers Look for Sales and Promotions?
Knowing when to buy can save you a lot of money on oxygen machines. Here are some key times to look for sales and promotions:
Major Holidays
Holidays like Black Friday, Cyber Monday, and Memorial Day are great opportunities to find significant discounts on oxygen machines from medical equipment retailers. During these times, you can expect savings ranging from 10% to 30% off regular prices.
Seasonal Clearance Events
Medical supply companies often have clearance events when new models come out. This is when they discount older models to make room for the new ones. If you’re looking for a budget-friendly option, this is a good time to buy as you can get quality equipment at reduced rates without sacrificing functionality.
Promotional Offers
In addition to price reductions, some retailers offer promotional offers that include valuable services with your purchase. These offers can include:
- Free pulmonary rehabilitation courses (valued at $200-$500)
- Extended warranty coverage at no additional cost
- Complimentary maintenance kits including filters and tubing
- No-interest financing for qualified buyers
These incentives not only save you money but also improve your health outcomes by providing professional guidance on managing your oxygen …
Read MoreMedical Oxygen at Home: Essential Information on Oxygen Tanks, Machines, and Therapies
Introduction
For individuals with chronic respiratory conditions, such as COPD, asthma, or emphysema, medical oxygen therapy at home is often a critical part of maintaining health and improving quality of life. Whether you need an oxygen machine for home, oxygen tank, or oxygen concentrator, choosing the right equipment is essential for your health management. In this guide, we will cover everything you need to know about medical oxygen supplies, including the different types of devices available, how they work, and how to choose the best option for your home oxygen therapy needs in Australia.
What is Medical Oxygen?
Medical oxygen is a vital treatment for individuals with respiratory conditions who are unable to maintain normal oxygen levels in their blood. It can be delivered through different devices, such as oxygen tanks, home oxygen concentrators, and oxygen generators for home use. The purpose of oxygen therapy at home is to ensure that patients receive a continuous and reliable supply of oxygen to improve breathing, prevent complications, and enhance overall health.
Types of Oxygen Devices for Home Use
There are several types of oxygen devices available for home use, each designed to meet specific needs. Choosing the right device depends on factors such as the patient’s oxygen requirements, mobility, and lifestyle.
1. Oxygen Tanks for Home Use
Oxygen tanks are the most traditional and commonly used method for delivering medical oxygen. These tanks store oxygen in a compressed or liquid form and are available in various sizes. Oxygen tanks for breathing at home typically require regular refills, which can be done through home delivery services or at medical supply stores.
- Pros: Portable, widely available, and easy to use.
- Cons: Requires regular refills, which can be inconvenient. Also, tanks have a limited supply of oxygen and must be replaced once depleted.
2. Home Oxygen Concentrators
A home oxygen concentrator is a medical device that extracts oxygen from the air and delivers concentrated oxygen to patients who need it. Unlike oxygen tanks, home oxygen concentrators do not require refills and can provide an endless supply of oxygen as long as they are plugged into a power source.
- Pros: No need for regular refills, continuous oxygen supply.
- Cons: Larger and less portable than oxygen tanks, typically require a constant power source.
3. Oxygen Generators for Home Use
An oxygen generator for home use is a more advanced solution that works similarly to a concentrator, but it is designed to provide a higher volume of oxygen. This type of device separates nitrogen from the air and delivers pure oxygen to the user. They are commonly used for patients with higher oxygen needs.
- Pros: High oxygen output, continuous supply.
- Cons: Larger and more expensive than standard oxygen concentrators.
4. Portable Oxygen Concentrators
For patients who require more mobility, portable oxygen concentrators are a great option. These devices are lightweight and designed to be carried around, making them ideal for patients who are active and need oxygen at home but also want the flexibility to travel.
- Pros: Portable, lightweight, ideal for travel.
- Cons: Limited battery life, typically lower oxygen output than stationary concentrators.
5. Oxygen Masks and Cannulas
For delivering medical oxygen, oxygen masks for home use or nasal cannulas are essential accessories. An oxygen mask for home is used for patients who require a higher flow of oxygen, while nasal cannulas are ideal for those who need lower amounts of oxygen. These accessories are typically connected to oxygen tanks or oxygen machines for home use.
- Pros: Easy to use, comfortable.
- Cons: Must be replaced regularly for hygiene purposes.
How Does Oxygen Therapy at Home Work?
Oxygen therapy at home works by delivering oxygen air to patients who need it to maintain healthy oxygen levels in their blood. The treatment can be administered through oxygen concentrators, oxygen tanks, or oxygen compressors, depending on the patient’s needs and the severity of their condition.
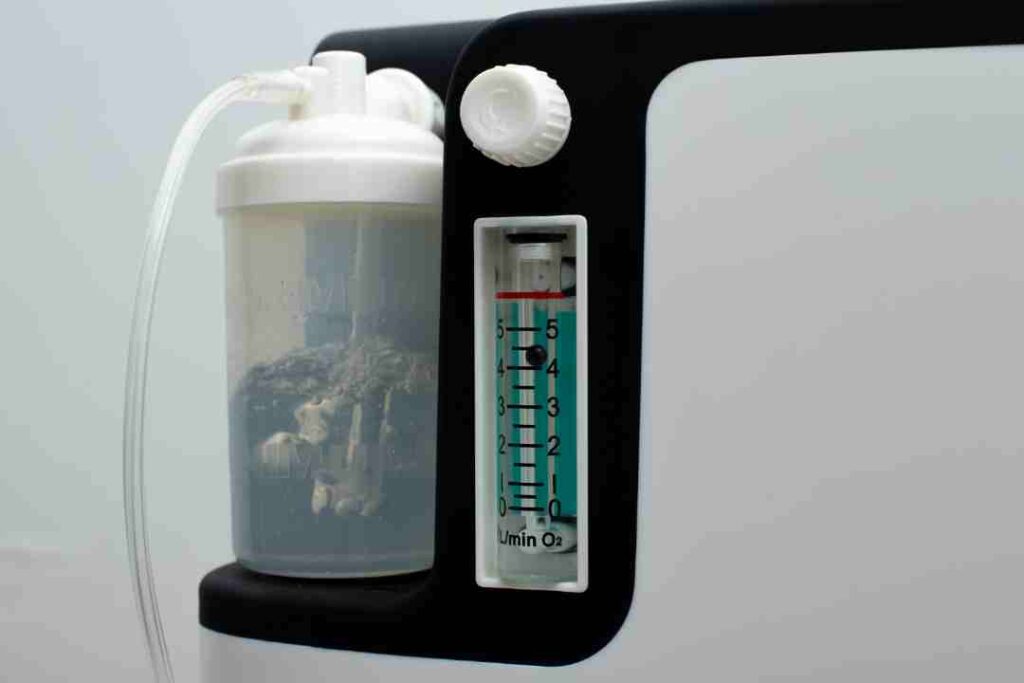
1. Determining Oxygen Flow Rates
Oxygen flow rates are typically measured in liters per minute (LPM). Depending on your healthcare provider’s recommendation, the oxygen flow rate may vary. Some patients require a continuous flow of oxygen, while others may only need pulse dose oxygen, which is delivered when the patient inhales. This is where devices like Philips EverFlo or Inogen One come into play, as they offer both continuous and pulse flow options.
2. Oxygen Mask or Nasal Cannula
The oxygen mask for home use or nasal cannula is connected to the oxygen source and is placed over the patient’s nose and mouth (for the mask) or just in the nostrils (for the cannula). The oxygen supply is then delivered to the patient in a steady stream, ensuring that the body receives the necessary oxygen for breathing and overall health.
How Much Does Oxygen Cost?
The cost of medical oxygen depends on the type of device and the supplier. Oxygen tank prices can range from AUD 150 to AUD 500 depending on the size and type, while home oxygen concentrators generally cost between AUD 2,500 to AUD 5,000. Portable oxygen concentrators typically cost between AUD 3,000 and AUD 6,000, depending on the brand and features.
Additionally, oxygen therapy at home may come with ongoing costs, such as regular oxygen tank refills or maintenance for devices like oxygen concentrators. It’s important to consider these ongoing costs when deciding on the right oxygen machine for home.
Where to Buy Oxygen Machines for Home Use in Australia
There are several options for buying oxygen machines for home use in Australia. Some of the most trusted suppliers include:
- Oxygen Australia: Offers a range of oxygen concentrators, portable oxygen machines, and medical oxygen supplies.
- Lincare Australia: Known for providing high-quality oxygen equipment and services across Australia.
- Air Liquide Home Oxygen: Specializes in providing oxygen tanks for breathing at home and oxygen concentrators for purchase or rent.
- Pharmacy Direct: Offers various oxygen machines for home use, including home oxygen concentrators and accessories.
Conclusion
Choosing the right oxygen machine for home use is crucial for individuals who require oxygen therapy at home. Whether you opt for a portable oxygen concentrator, oxygen tank, or a home oxygen concentrator, it’s important to consider factors like oxygen flow rate, portability, and cost. By understanding the different medical oxygen devices available and their features, you can make an informed decision that will improve your health and well-being. Always consult with your healthcare provider to ensure the right device is selected for your specific needs.
… Read MoreUnderstanding Sleep Apnea: Causes, Symptoms, and Effective Treatments
Sleep is one of the most vital pillars of good health, but for millions of people, restful sleep is harder to achieve than it should be. One of the most common reasons for poor sleep quality is sleep apnea, a potentially serious sleep disorder that often goes undiagnosed.
If you’ve ever been told you snore loudly, gasp for air during sleep, or feel unusually tired during the day, sleep apnea might be the cause. In this article, we’ll explore what sleep apnea is, its causes, symptoms, and the most effective treatment options — from simple lifestyle changes to advanced therapies.
What Is Sleep Apnea?
Sleep apnea is a sleep disorder where a person’s breathing repeatedly stops and starts during sleep. These pauses can last from a few seconds to a minute and may occur dozens of times throughout the night.
There are three main types of sleep apnea:
- Obstructive Sleep Apnea (OSA) – The most common type, caused by blockage of the airway due to relaxed throat muscles.
- Central Sleep Apnea (CSA) – Occurs when the brain fails to send the proper signals to muscles controlling breathing.
- Complex or Mixed Sleep Apnea – A combination of both obstructive and central sleep apnea.
Regardless of the type, the result is the same — disrupted sleep and reduced oxygen levels that can impact overall health.
The Hidden Dangers of Sleep Apnea
While many people dismiss snoring as harmless, untreated sleep apnea can lead to serious health complications, including:
- High blood pressure and heart disease
- Stroke or irregular heart rhythms
- Type 2 diabetes
- Chronic fatigue and mood disorders
- Cognitive decline and memory problems
When breathing repeatedly stops during the night, oxygen levels drop, forcing the heart and brain to work harder. Over time, this strain can significantly increase the risk of cardiovascular and metabolic diseases.
Common Causes of Sleep Apnea
Sleep apnea can affect anyone, but certain factors increase your risk. Here are the most common causes and risk factors:
1. Excess Weight
Carrying extra fat around the neck can narrow the airway, making it harder to breathe at night. Obesity is one of the leading causes of obstructive sleep apnea.
2. Anatomical Factors
Some people naturally have smaller airways, enlarged tonsils, or a thick neck structure, which can restrict airflow during sleep.
3. Age and Gender
Sleep apnea is more common in men and tends to increase with age, although women are also at risk, especially after menopause.
4. Family History
A family history of sleep apnea can increase your chances of developing the condition, particularly if similar facial or airway structures are inherited.
5. Lifestyle Habits
Smoking, alcohol consumption, and sedative use relax throat muscles, making airway collapse more likely during sleep.
6. Medical Conditions
Certain conditions like nasal congestion, hypothyroidism, and neuromuscular disorders can contribute to airway obstruction or irregular breathing patterns.
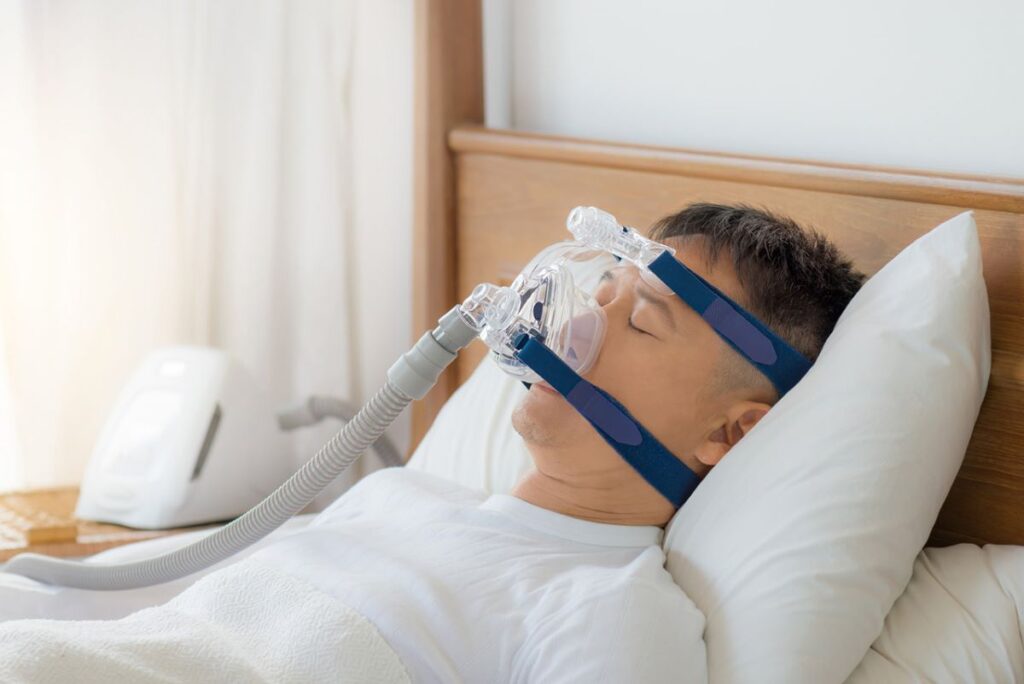
Recognizing the Symptoms of Sleep Apnea
Sleep apnea often goes undetected because the person affected may not remember waking up throughout the night. However, common symptoms include:
- Loud, chronic snoring
- Pauses in breathing observed by a partner
- Gasping or choking during sleep
- Daytime fatigue or falling asleep during routine activities
- Morning headaches
- Irritability, mood swings, or depression
- Poor concentration and memory problems
If you or your partner notice these signs, it’s important to consult a doctor or sleep specialist for further evaluation.
Diagnosing Sleep Apnea: The Role of Sleep Studies
A sleep study (also known as polysomnography) is the gold standard for diagnosing sleep apnea. This test can be done either at a sleep clinic or through an at-home sleep test.
In-Lab Sleep Study
During a clinic-based sleep study, sensors are attached to monitor:
- Breathing patterns
- Brain activity (EEG)
- Oxygen levels
- Heart rate
- Leg and eye movements
At-Home Sleep Test
For mild to moderate cases, doctors may recommend a simplified home-based version that records breathing, oxygen, and airflow data overnight.
Both methods help determine the severity of sleep apnea and guide treatment options.
Effective Treatments for Sleep Apnea
Treatment depends on the type and severity of your sleep apnea, but the goal is always the same — to keep your airway open and improve oxygen flow during sleep. Let’s explore the most effective options.
1. CPAP Therapy (Continuous Positive Airway Pressure)
The CPAP machine is the most common and effective treatment for obstructive sleep apnea. It delivers a steady stream of air through a mask, preventing airway collapse.
Benefits of CPAP therapy:
- Reduces snoring and daytime sleepiness
- Improves sleep quality and energy levels
- Decreases the risk of heart disease and high blood pressure
Though it can take time to adjust, most users experience significant improvement within days.
2. Oral Appliances
For mild to moderate sleep apnea, oral appliances are a great alternative to CPAP. These custom-fitted devices reposition the jaw and tongue to keep the airway open.
They’re ideal for people who travel frequently or find CPAP masks uncomfortable.
3. Lifestyle Modifications
Simple lifestyle changes can have a big impact on managing sleep apnea symptoms:
- Lose excess weight to reduce pressure on the airway
- Sleep on your side instead of your back
- Avoid alcohol and sedatives before bedtime
- Quit smoking, as it increases inflammation and airway swelling
- Maintain a regular sleep schedule
4. Surgery
In severe or treatment-resistant cases, surgery may be recommended to remove or reduce tissue blocking the airway. Common procedures include uvulopalatopharyngoplasty (UPPP), nasal surgery, or jaw repositioning.
5. Emerging Treatments
Modern medicine continues to advance sleep apnea care. Inspire therapy, a newer treatment, uses a small implanted device that stimulates airway muscles to prevent collapse — offering a high-tech alternative to traditional methods.
Living Well with Sleep Apnea
Managing sleep apnea isn’t just about better sleep — it’s about improving your quality of life. With the right treatment and lifestyle changes, most people experience:
- More energy and alertness
- Improved mood and focus
- Lower risk of heart problems
- Better relationships due to reduced snoring and restlessness
Early diagnosis and consistent treatment can make a world of difference.
Final Thoughts
Sleep apnea is more than just loud snoring — it’s a serious medical condition that affects your overall health and well-being. The good news is that with the right approach — from CPAP therapy and oral appliances to lifestyle changes — it’s completely manageable.
If you suspect you or a loved one has sleep apnea, talk to a sleep specialist and consider getting a sleep study. The sooner you act, the sooner you can reclaim restful, healthy sleep.
FAQS
Sleep apnea is often caused by airway obstruction during sleep, excess weight, nasal congestion, or anatomical issues in the throat. It can also result from neurological conditions that disrupt breathing signals between the brain and body.
Common symptoms include loud snoring, choking or gasping during sleep, daytime fatigue, morning headaches, and difficulty concentrating. If left untreated, sleep apnea can lead to more serious health problems like heart disease or high blood pressure.
A sleep specialist usually diagnoses sleep apnea through an overnight sleep study (polysomnography) or a home-based sleep test. These tests record your breathing patterns, oxygen levels, and heart rate to identify the severity of your sleep disorder.
Treatment options include CPAP therapy, oral appliances, lifestyle changes (like losing weight or avoiding alcohol), and in severe cases, surgery. The right approach depends on the type and severity of your sleep apnea.
Bulk-Bill Sleep Study Brisbane: Affordable Options for Locals
What Are Bulk-Bill Sleep Studies and How Do They Work in Brisbane?
Bulk-bill sleep study Brisbane services provide you with direct billing to Medicare, eliminating upfront costs for diagnostic testing. When you receive a bulk-bill sleep study, the healthcare provider charges Medicare directly under the Medicare Benefits Schedule (MBS), meaning you pay nothing out-of-pocket for eligible services.
Home sleep study Brisbane options have transformed how sleep disorders are diagnosed by bringing testing directly to your bedroom. Here’s how it typically works:
- Equipment delivery: The necessary devices are brought to your home, along with easy-to-follow instructions on how to set them up.
- Non-invasive monitoring: These devices are designed to be non-intrusive, meaning they won’t disrupt your sleep. They will monitor important factors such as your breathing patterns, oxygen levels, and sleep position.
- Overnight recording: The actual testing takes place overnight while you sleep in your own comfortable environment.
- Equipment collection: The next day, the equipment is picked up for analysis of the collected data.
Understanding Eligibility for Medicare Bulk Billing
To qualify for Medicare bulk billing, certain clinical criteria must be met and proper referral pathways followed. This means that you need to have a referral from either your GP or a sleep specialist who has evaluated your symptoms using approved screening methods.
The Medicare Benefits Schedule provides coverage for diagnostic sleep studies as long as they adhere to established medical guidelines.
How Sleep Data is Analysed
Once the data has been collected, it is examined by certified sleep physicians who interpret the results remotely. This efficient process helps to reduce waiting times while still ensuring accurate diagnoses.
The Advantages of Bulk-Bill Sleep Studies
The definition of a bulk-bill sleep study includes comprehensive overnight monitoring without the hassle and cost associated with traditional in-laboratory testing. This makes it easier for more residents in Brisbane to get diagnosed with sleep disorders and seek treatment promptly, something that might not have been possible otherwise.
Who Qualifies for a Bulk-Billed Sleep Study in Brisbane?
Eligibility for bulk billing, which allows patients to access subsidised sleep studies, requires you to meet specific medical and administrative criteria. Your journey begins with obtaining a referral from your GP or a specialist such as a respiratory physician, cardiologist, or ENT surgeon. These healthcare professionals assess your symptoms and determine whether you require diagnostic testing for sleep disorders.
The Epworth Sleepiness Scale (ESS) serves as a primary screening tool to evaluate your daytime sleepiness levels. You’ll complete this questionnaire rating how likely you are to doze off in various situations, from watching television to sitting in traffic. Scores above 10 typically indicate excessive daytime sleepiness warranting further investigation.
Healthcare providers also utilise the OSA50 score criteria to assess your risk of obstructive sleep apnea. This screening tool evaluates factors including:
- Your neck circumference and BMI
- Age and gender demographics
- Presence of high blood pressure
- Snoring frequency and intensity
- Witnessed breathing interruptions during sleep
To qualify for the bulk-billed sleep study, you must demonstrate clinical symptoms such as loud snoring, breathing cessations, morning headaches, or excessive fatigue. Your referring doctor will document these symptoms alongside your screening scores to establish medical necessity. It’s important to note that private health insurance status doesn’t affect your eligibility – the assessment focuses purely on clinical need and Medicare guidelines.
Meeting these clinical thresholds ensures you receive appropriate diagnostic testing while maintaining the integrity of the bulk-billing system for those who genuinely require sleep disorder evaluation.
Which Providers Offer Bulk-Billed Sleep Studies in Brisbane?
Brisbane residents have access to several established sleep study providers Brisbane that facilitate bulk-billed diagnostic testing through strategic partnerships and Medicare-compliant services.
Air Liquide Healthcare stands as Australia’s largest facilitator of home sleep apnoea studies, operating an extensive network that covers Brisbane and surrounding areas. Their comprehensive approach includes partnerships with leading CPAP equipment manufacturers, ensuring patients receive integrated care from diagnosis through treatment initiation.
The company operates through multiple recognised brands including:
- SNORE Australia – specialising in sleep disorder diagnostics
- Healthy Sleep Solutions – focusing on therapeutic interventions
- Mycroft and Complete Care – providing comprehensive sleep medicine services
- Sleep Disorder Australia (SDCA) – offering specialised clinical support
ResMed stores Brisbane locations provide direct access to sleep technology and often coordinate with bulk-billing providers for seamless patient pathways. These facilities typically offer equipment demonstrations and initial consultations.
Sleep Solutions Australia operates several clinics across Brisbane, many offering extended hours to accommodate working patients. Their home-based study options eliminate the need for overnight hospital stays whilst maintaining clinical accuracy.
Nexus Healthcare provides additional coverage through their network of affiliated sleep specialists and diagnostic centres, ensuring patients can access bulk-billed services regardless of their location within the greater Brisbane area.
Many providers offer after-hours clinics and flexible appointment scheduling, recognising that sleep disorders often affect individuals with demanding work schedules who require convenient testing options.

How Do Home Sleep Studies Benefit Patients Compared to In-Lab Studies?
Home sleep study benefits extend far beyond simple convenience, transforming how Brisbane residents access sleep disorder diagnosis. You can complete your assessment in your own bed, eliminating the anxiety and discomfort associated with sleeping in unfamiliar clinical environments. This familiar setting produces more accurate results as you maintain your regular sleep patterns and routines.
The non-invasive sleep testing technology used in home studies requires minimal equipment setup. You’ll receive a compact monitoring device that tracks:
- Breathing patterns and airflow
- Blood oxygen levels
- Heart rate variations
- Sleep position changes
- Chest and abdominal movement
Patient comfort sleep diagnosis becomes achievable without the wires, electrodes, and constant monitoring that characterise traditional sleep laboratories. You simply wear a small device overnight, allowing natural sleep cycles to occur without interruption from technicians or unfamiliar sounds.
Remote analysis by certified sleep physicians ensures diagnostic accuracy matches laboratory standards. Your overnight data transmits securely to qualified specialists who interpret results using the same clinical criteria applied in hospital settings. This process maintains diagnostic integrity while reducing costs significantly.
The technology captures essential sleep metrics without requiring expensive overnight facility stays. You avoid scheduling conflicts with work or family commitments, as home studies accommodate your preferred timing. Brisbane residents particularly benefit from this flexibility, accessing professional sleep disorder assessment without the traditional barriers of location, cost, or clinical availability constraints.
See Also : Sleep Apnea Test Adelaide: Early Diagnosis for Better Health
What Are the Steps in the Patient Pathway for Diagnosing and Managing Obstructive Sleep Apnea (OSA)?
The OSA diagnosis pathway in Brisbane follows a structured approach that ensures patients receive comprehensive care from initial assessment through long-term management. Your journey begins when your GP or specialist identifies potential sleep apnea symptoms and provides a referral for testing.
The Complete Patient Journey
Step 1: Initial Assessment and Home Study
You’ll receive a home sleep study device that monitors your breathing patterns, oxygen levels, and sleep quality overnight. This non-invasive approach eliminates the need for hospital stays whilst providing accurate diagnostic data.
Step 2: Results Analysis and Diagnosis
Certified sleep physicians analyse your study results remotely, determining the severity of your OSA and recommending appropriate treatment options based on clinical findings.
Step 3: Treatment Initiation
Upon diagnosis, CPAP therapy initiation Brisbane services connect you with appropriate equipment and initial setup support. Local providers like Air Liquide Healthcare facilitate this process through partnerships with major CPAP manufacturers.
Step 4: Titration and Optimisation
CPAP titration programs help determine your optimal pressure settings through either additional home studies or auto-titrating devices that adjust throughout the night.
Step 5: Ongoing Support and Monitoring
Therapy management sleep apnea includes regular follow-ups, equipment maintenance guidance, and continuous support from sleep coaches. This ensures your treatment remains effective and comfortable long-term, with adjustments made as needed to maintain optimal therapeutic outcomes.
How Does Medicare Support Bulk-Bill Sleep Studies and CPAP Therapy Costs?
Medicare coverage sleep studies operates through the Medicare Benefits Schedule (MBS), which provides specific item numbers for sleep disorder diagnostic tests. The MBS guidelines diagnostic tests require patients to meet clinical criteria and obtain appropriate referrals from qualified medical practitioners. You can access bulk-billed sleep studies when your GP or specialist determines you meet the necessary medical requirements outlined in these guidelines.
The diagnostic phase receives comprehensive Medicare support, covering home-based sleep monitoring equipment and professional interpretation by certified sleep physicians. This means you won’t face out-of-pocket expenses for the initial assessment when providers offer bulk-billing services.
Private health insurance CPAP coverage varies significantly between insurers and policy types. Many private health funds include CPAP equipment and ongoing therapy costs under their extras or hospital cover packages. You should verify your specific policy details, as coverage levels differ:
- Gold-tier hospital cover typically includes comprehensive sleep disorder benefits
- Extras packages may cover CPAP equipment rental or purchase
- Waiting periods often apply before you can claim benefits
When you don’t qualify for bulk-billing, several alternatives exist. Some providers offer payment plans or reduced-fee consultations for eligible patients. Air Liquide Healthcare’s network partners frequently provide flexible payment options, ensuring access to essential sleep disorder services …
Read MoreSleep Apnea Test Adelaide: Early Diagnosis for Better Health
What Is Sleep Apnea and Why Is Early Diagnosis Important?
Sleep apnea is a serious sleep disorder where your breathing repeatedly stops and starts during sleep. This condition affects millions of people worldwide, yet many remain undiagnosed, missing crucial opportunities for intervention that could dramatically improve their health outcomes.
Obstructive Sleep Apnea (OSA) is the most common form of this condition. During OSA episodes, your throat muscles relax excessively, causing the airway to narrow or close completely. This blockage prevents adequate airflow, forcing your brain to wake you briefly to restore normal breathing. These interruptions can occur hundreds of times per night, severely fragmenting your sleep quality.
The health consequences of untreated sleep apnea extend far beyond daytime fatigue:
- Cardiovascular complications including high blood pressure, heart disease, and stroke
- Type 2 diabetes development due to insulin resistance
- Depression and anxiety stemming from chronic sleep deprivation
- Cognitive impairment affecting memory, concentration, and decision-making abilities
Early diagnosis through a sleep apnea test Adelaide services provide can be life-changing. When you identify and treat sleep apnea promptly, you significantly reduce your risk of developing these serious health complications. Better health outcomes become achievable through proper treatment, leading to improved energy levels, enhanced cognitive function, and reduced cardiovascular risks.
You deserve restorative sleep that supports your long-term wellbeing. Early diagnosis empowers you to take control of your health before complications develop, making the investment in professional sleep testing invaluable for your future quality of life.
How Is Sleep Apnea Tested in Adelaide?
Adelaide residents have access to two primary sleep apnea testing methods that cater to different patient needs and preferences. You can choose between comprehensive in-clinic overnight studies conducted in specialised sleep laboratories or convenient home-based sleep studies that allow testing in your familiar environment.
In-clinic Sleep Study
In-clinic sleep study Adelaide facilities provide the most comprehensive diagnostic approach. These overnight studies, known as polysomnography, monitor multiple physiological parameters simultaneously:
- Brain wave activity through electroencephalography (EEG)
- Eye movements via electrooculography (EOG)
- Muscle tension measurements using electromyography (EMG)
- Heart rhythm monitoring with electrocardiography (ECG)
- Respiratory airflow and effort sensors
- Blood oxygen saturation monitors
- Body position sensors
Home Sleep Study
Home sleep study Adelaide options utilise portable monitoring devices that focus on essential respiratory parameters. These non-invasive recording systems typically include:
- Nasal airflow sensors
- Chest and abdominal effort belts
- Pulse oximetry for oxygen levels
- Body position monitors
The testing environments differ significantly in their approach. Clinic-based studies offer controlled conditions with immediate technical support and comprehensive monitoring capabilities. Home studies provide the comfort of your own bedroom whilst maintaining diagnostic accuracy for obstructive sleep apnea detection. Both methods collect crucial data that sleep specialists analyse to determine the presence and severity of sleep-disordered breathing patterns.
Who Provides Sleep Apnea Testing Services in Adelaide?
Air Liquide Healthcare is Australia’s largest provider of home sleep apnea studies and therapy, making it the leading choice for sleep clinics in Adelaide. What sets them apart is their comprehensive approach, offering solutions that cover diagnosis, treatment, and ongoing management of obstructive sleep apnea with the approval of certified sleep physicians.
The company’s wide-ranging network operates through strategic partnerships with CPAP equipment manufacturers, ensuring patients have access to the latest therapeutic technologies. This extensive coverage includes several well-known sleep brands across Adelaide:
- SNORE Australia – Specialising in comprehensive sleep disorder solutions
- Healthy Sleep Solutions – Focused on patient-centred care approaches
- Mycroft – Providing clinical expertise and equipment support
- Complete Care – Offering holistic sleep health management
- Sleep Disorder Australia (SDCA) – Delivering specialised diagnostic services
Certified sleep physicians are essential in validating diagnoses and treatment protocols for all these providers. These medical professionals guarantee that each patient receives clinically appropriate care based on their specific sleep study results. You can expect these specialists to thoroughly review your test data, confirm diagnostic accuracy, and recommend the most suitable treatment pathway for your individual needs.
The collaborative effort between Air Liquide Healthcare and its partner brands establishes a strong support network that upholds consistent quality standards while offering you convenient access to sleep apnea testing services throughout Adelaide’s metropolitan area.
What Does the Patient Pathway Look Like for Sleep Apnea Testing?
The patient pathway sleep apnea process begins with an initial consultation where you discuss your symptoms, medical history, and sleep patterns with a qualified healthcare professional. During this assessment, specialists evaluate factors such as snoring frequency, daytime fatigue, and observed breathing interruptions to determine if sleep testing is necessary.
Study Administration Options
You have two primary testing environments available:
- Home-based studies – Non-invasive recording devices monitor your breathing patterns, oxygen levels, and sleep position in your familiar bedroom environment
- Clinic-based studies – Comprehensive overnight monitoring in a controlled medical facility with additional sensors and real-time observation
Analysis and Follow-up Process
Sleep physicians analyse your test data within 7-10 days, examining breathing events, oxygen saturation levels, and sleep architecture patterns. You receive detailed results during a follow-up consultation where specialists explain your diagnosis to treatment process and discuss appropriate management strategies.
CPAP Therapy Initiation
When sleep apnea is confirmed, CPAP therapy initiation begins with equipment fitting and pressure titration programs. You receive comprehensive training on device operation, mask selection, and maintenance procedures. Ongoing support includes regular check-ups to monitor treatment effectiveness, adjust pressure settings, and address any compliance challenges you might experience.
This structured approach ensures you receive personalised care throughout your journey, from initial symptoms to effective treatment management.

How Do Medicare and Private Insurance Support Sleep Apnea Testing in Adelaide?
Medicare coverage sleep studies provide significant financial relief for Adelaide residents seeking sleep apnea diagnosis. The Australian government recognises sleep disorders as legitimate medical conditions, offering bulk-billing options for diagnostic tests that meet MBS guidelines. You can access these services without upfront costs when providers comply with Medicare Benefits Schedule requirements, making initial testing accessible regardless of your financial situation.
Sleep study providers in Adelaide work directly with Medicare to streamline the billing process. You’ll typically receive bulk-billed services for:
- Initial sleep physician consultations
- Home-based sleep study equipment and monitoring
- Follow-up appointments for result discussions
- Specialist referrals when required
Private insurance CPAP therapy coverage varies significantly between insurers and policy levels. Many private health funds include sleep disorder treatments under their hospital or extras cover packages. You might find CPAP equipment, masks, and ongoing therapy support covered under specific tiers of private health insurance.
The coverage landscape requires careful navigation. Each insurer maintains different criteria for sleep apnea treatment benefits, with some requiring prior approval or specialist recommendations. You should contact your private health fund directly to understand your specific entitlements and any waiting periods that might apply.
Checking your eligibility before commencing treatment prevents unexpected costs. Adelaide sleep clinics often assist patients in verifying insurance coverage, ensuring you understand your financial responsibilities upfront and can plan your treatment journey accordingly. Click here to get more about Bulk-Bill Sleep Study Brisbane.
What Are the Benefits of Home-Based Sleep Studies Compared to In-Clinic Tests?
Home sleep study advantages extend far beyond simple convenience, offering patients a more natural and comfortable testing environment. When you conduct a sleep study in your own bedroom, you eliminate the anxiety and unfamiliarity that often accompanies overnight clinic stays. This familiar setting allows for more representative sleep patterns, potentially leading to more accurate diagnostic results.
The convenience of home testing transforms the entire diagnostic experience. You can maintain your regular bedtime routine, sleep in your own bed, and avoid the disruption of travelling to and from a sleep clinic. This approach particularly benefits patients with mobility issues, busy schedules, or those who feel uncomfortable sleeping away from home.
Modern portable monitoring devices used in home studies are remarkably sophisticated yet user-friendly. These non-invasive recording systems typically include:
- Chest and abdominal effort belts to monitor breathing patterns
- Nasal airflow sensors to detect breathing interruptions
- Pulse oximeters to measure blood oxygen levels
- Position sensors to track sleep posture
The accuracy of portable monitoring relies heavily on proper patient education and support. Adelaide’s leading sleep study providers ensure you receive comprehensive instructions on device placement and operation. Many services include video tutorials and 24-hour support hotlines to address any concerns during your study night.
Patient education programmes help you understand the importance of following normal sleep routines whilst wearing the monitoring equipment, ensuring the collected data accurately reflects your typical sleep patterns.
How Do Sleep Clinics Ensure Patient Comfort and Support During Testing?
Patient comfort during sleep testing is a top priority for Adelaide’s leading sleep clinics. These clinics have specialised teams who focus on your wellbeing throughout the entire diagnostic process. They understand that undergoing testing can be overwhelming, so they have implemented comprehensive support systems tailored to your specific needs.
Support from the Beginning
The patient-centered approach starts from your very first consultation. During this meeting, certified sleep technicians will take the time to explain each step of the process in detail. Whether you’re participating in home-based studies or clinic testing, you will receive clear instructions on how to use the equipment. This educational foundation aims to …
Read MoreRecent Posts
 Home vs. Portable: Can One Oxygen Concentrator Do Both?Home vs. Portable: Can One Oxygen Concentrator Do Both? For many Australians managing chronic respiratory conditions like COPD or emphysema, the quest for the "perfect" oxygen setup often leads to one critical question: Can one oxygen concentrator do […]
Home vs. Portable: Can One Oxygen Concentrator Do Both?Home vs. Portable: Can One Oxygen Concentrator Do Both? For many Australians managing chronic respiratory conditions like COPD or emphysema, the quest for the "perfect" oxygen setup often leads to one critical question: Can one oxygen concentrator do […] Understanding Your Sleep Study Report: What the Results MeanThis guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician. What is a sleep study report actually measuring? A sleep study report explains how they sleep and how their […]
Understanding Your Sleep Study Report: What the Results MeanThis guide explains what those results typically mean, so they can follow the logic of the report before discussing next steps with a clinician. What is a sleep study report actually measuring? A sleep study report explains how they sleep and how their […] Sleep Apnea Test Adelaide: 5 Signs You Should Book OneIf they live in Adelaide and recognise the signs below, booking a sleep apnoea test is often the fastest way to get clarity and start feeling better. What exactly is sleep apnoea, and why does testing matter? A sleep apnea test Adelaide service is used […]
Sleep Apnea Test Adelaide: 5 Signs You Should Book OneIf they live in Adelaide and recognise the signs below, booking a sleep apnoea test is often the fastest way to get clarity and start feeling better. What exactly is sleep apnoea, and why does testing matter? A sleep apnea test Adelaide service is used […] Ultimate Guide to Choosing an Oxygen Concentrator in Australia (2026)ntroduction to Modern Oxygen Therapy For many Australians living with chronic respiratory conditions, maintaining an active lifestyle in cities like Sydney requires more than just medical advice—it requires the right technology. An oxygen concentrator is […]
Ultimate Guide to Choosing an Oxygen Concentrator in Australia (2026)ntroduction to Modern Oxygen Therapy For many Australians living with chronic respiratory conditions, maintaining an active lifestyle in cities like Sydney requires more than just medical advice—it requires the right technology. An oxygen concentrator is […] The Best CPAP Mask Options for New Users and What Makes Them ComfortableSleep apnea disrupts breathing during sleep, causing repeated pauses that prevent restful sleep and strain the cardiovascular system. CPAP therapy delivers continuous pressurized air through a mask, keeping airways open throughout the night and enabling […]
The Best CPAP Mask Options for New Users and What Makes Them ComfortableSleep apnea disrupts breathing during sleep, causing repeated pauses that prevent restful sleep and strain the cardiovascular system. CPAP therapy delivers continuous pressurized air through a mask, keeping airways open throughout the night and enabling […] Oxygen Machine for Home Use: A Complete Guide for First-Time BuyersWhat Is an Oxygen Machine and How Does It Work? An oxygen machine for home use, commonly known as an oxygen concentrator, is a medical device that delivers concentrated oxygen to individuals with respiratory conditions. These respiratory therapy devices […]
Oxygen Machine for Home Use: A Complete Guide for First-Time BuyersWhat Is an Oxygen Machine and How Does It Work? An oxygen machine for home use, commonly known as an oxygen concentrator, is a medical device that delivers concentrated oxygen to individuals with respiratory conditions. These respiratory therapy devices […] Medical Oxygen at Home: Essential Information on Oxygen Tanks, Machines, and TherapiesIntroduction For individuals with chronic respiratory conditions, such as COPD, asthma, or emphysema, medical oxygen therapy at home is often a critical part of maintaining health and improving quality of life. Whether you need an oxygen machine for […]
Medical Oxygen at Home: Essential Information on Oxygen Tanks, Machines, and TherapiesIntroduction For individuals with chronic respiratory conditions, such as COPD, asthma, or emphysema, medical oxygen therapy at home is often a critical part of maintaining health and improving quality of life. Whether you need an oxygen machine for […] Understanding Sleep Apnea: Causes, Symptoms, and Effective TreatmentsSleep is one of the most vital pillars of good health, but for millions of people, restful sleep is harder to achieve than it should be. One of the most common reasons for poor sleep quality is sleep apnea, a potentially serious sleep disorder that often […]
Understanding Sleep Apnea: Causes, Symptoms, and Effective TreatmentsSleep is one of the most vital pillars of good health, but for millions of people, restful sleep is harder to achieve than it should be. One of the most common reasons for poor sleep quality is sleep apnea, a potentially serious sleep disorder that often […] Bulk-Bill Sleep Study Brisbane: Affordable Options for LocalsWhat Are Bulk-Bill Sleep Studies and How Do They Work in Brisbane? Bulk-bill sleep study Brisbane services provide you with direct billing to Medicare, eliminating upfront costs for diagnostic testing. When you receive a bulk-bill sleep study, the […]
Bulk-Bill Sleep Study Brisbane: Affordable Options for LocalsWhat Are Bulk-Bill Sleep Studies and How Do They Work in Brisbane? Bulk-bill sleep study Brisbane services provide you with direct billing to Medicare, eliminating upfront costs for diagnostic testing. When you receive a bulk-bill sleep study, the […] Sleep Apnea Test Adelaide: Early Diagnosis for Better HealthWhat Is Sleep Apnea and Why Is Early Diagnosis Important? Sleep apnea is a serious sleep disorder where your breathing repeatedly stops and starts during sleep. This condition affects millions of people worldwide, yet many remain undiagnosed, missing […]
Sleep Apnea Test Adelaide: Early Diagnosis for Better HealthWhat Is Sleep Apnea and Why Is Early Diagnosis Important? Sleep apnea is a serious sleep disorder where your breathing repeatedly stops and starts during sleep. This condition affects millions of people worldwide, yet many remain undiagnosed, missing […]
Categories
- CPAP Machine
- CPAP Mask Online
- CPAP Masks
- Cpap Masks Australia
- Laser Eye Surgery
- Lasik Surgery
- Medical Oxygen
- Oxygen Concentrator
- Portable Oxygen Concentrator Australia
- Portable Oxygen Concentrator Machine
- ResMed AirMini
- Sleep Apnea
- Sleep Apnea Test Adelaide
- Sleep Apnea Test Brisbane
- Sleep Study
- Sleep Type Test
- Sydney Eye Clinic